AO Spine upper cervical injuries classification system
1. Preliminary remarks
The classification system described here exists in order to provide surgeons from different institutions with a common language to discuss various injuries. It provides consistency in injury diagnosis and treatment.
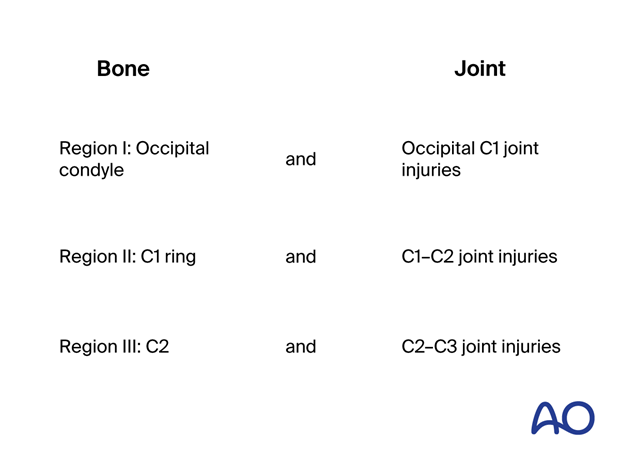
Unlike the subaxial, thoracolumbar, and sacral classifications, which have a uniform vertebral anatomy, the upper cervical spine has three distinct segments, with typical bones and joints. For this reason, this upper cervical area has been divided into three regions, as illustrated.
Each region involves a bone and its lower joint. In this way, it is possible to apply the morphological concepts already described in the A, B, C system to each one of the regions.
The AO Spine upper cervical injuries classification system aims to achieve international acceptance.
To make a diagnosis, imaging studies are required.
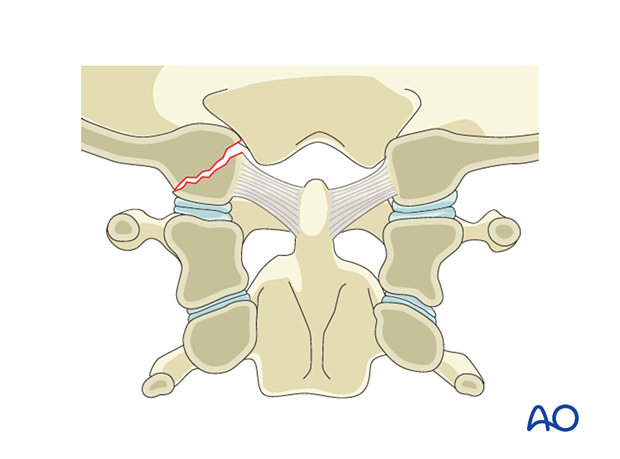
2. Region I: Occipital condyle and craniocervical junction - Type A: Isolated bony injury (condyle)
Type A injuries are any type of occipitocondyle fracture (simple or multifragmentary) without significant ligamentous injury.
These injuries are often stable, and nonoperative conservative management is most appropriate. A hard collar is indicated.
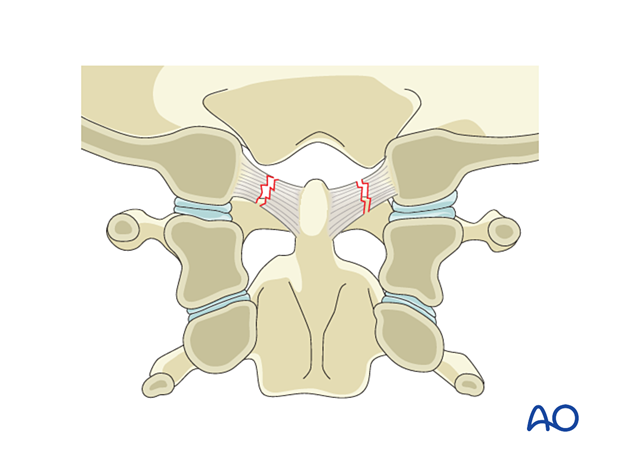
3. Region I: Occipital condyle and craniocervical junction - Type B: Nondisplaced ligamentous injury (craniocervical)
Type B injuries are nondisplaced ligamentous injuries with or without associated fractures of the occipital condyle. They are potentially unstable. A hard collar is indicated.
If a stress test shows displacement, it is considered a Type C injury.
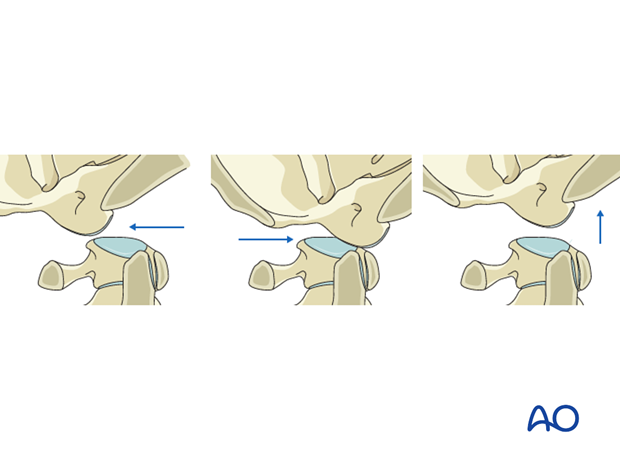
4. Region I: Occipital condyle and craniocervical junction - Type C: Any injury with displacement
Type C injuries are any injury with significant translation between the occiput and the cervical spine in any plane.
These injuries are very unstable, life-threatening, and often require urgent operative management.
Occipitocervical dissociation is typically the result of high-energy motor vehicle accidents. This is potentially fatal (mortality rate 50–60%).
Immediate diagnosis and treatment are crucial for a good outcome.
Diagnosis is made using CT imaging, and if there is any doubt about the diagnosis, MRI.
Those who survive will often present unconscious with a sign of a brain or spinal cord injury.
These injuries are treated with immediate stabilization in a halo device, followed by occipitocervical fusion as soon as possible.
5. Region II: C1 ring and C1–C2 joint - Type A: Isolated bony injury
Type A injuries are any C1 fracture (simple or multifragmentary) without significant ligamentous injury.
These may be fractures of the:
- Anterior arch
- Posterior arch
- Anterior and posterior arch
- Lateral mass
- Transverse process
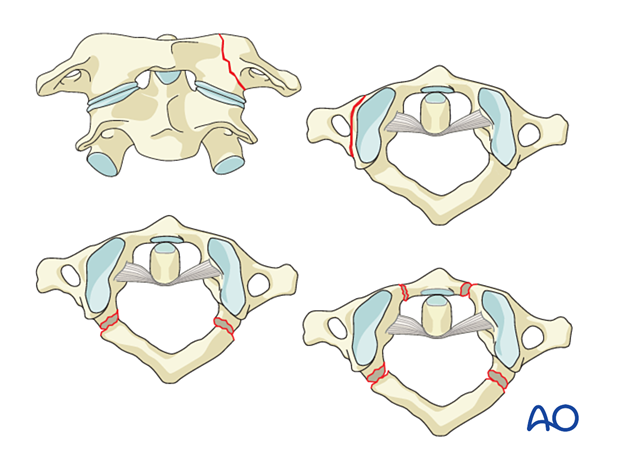
Anterior arch injury
Anterior arch injuries are in general hyperflexion injuries. These are normally stable and treated with no immobilization or use of a collar for pain management.
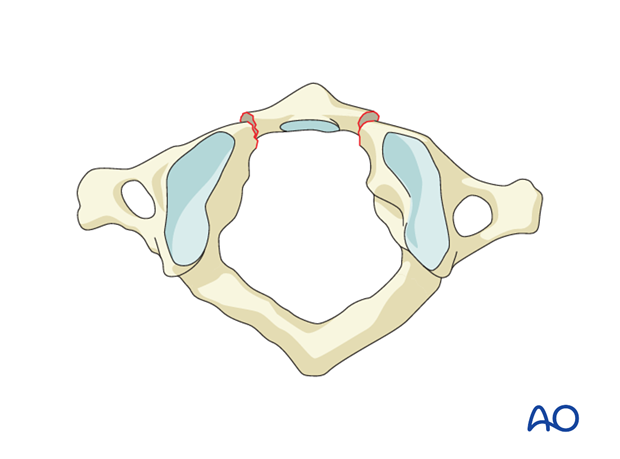
Posterior arch injury
Posterior arch injuries are hyperextension injuries. These are normally stable and treated with no immobilization or use of a collar for pain management.
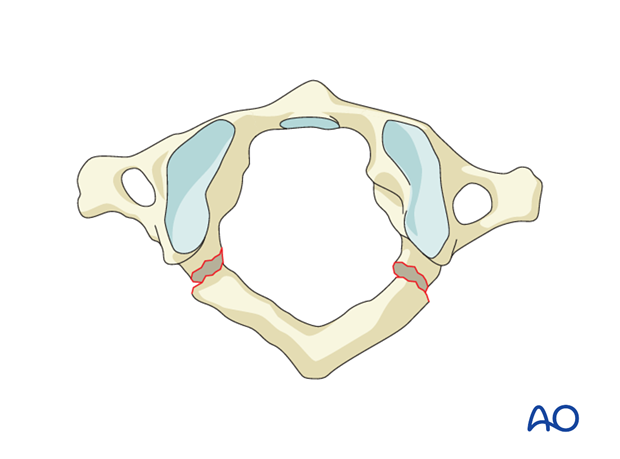
Combined posterior and anterior arch injury
Burst fractures are axial load injuries resulting in both anterior and posterior ring fractures. The fractures can be uni- or bilateral.
Nondisplaced burst fractures are normally treated nonoperatively without immobilization or use of a collar for pain management.
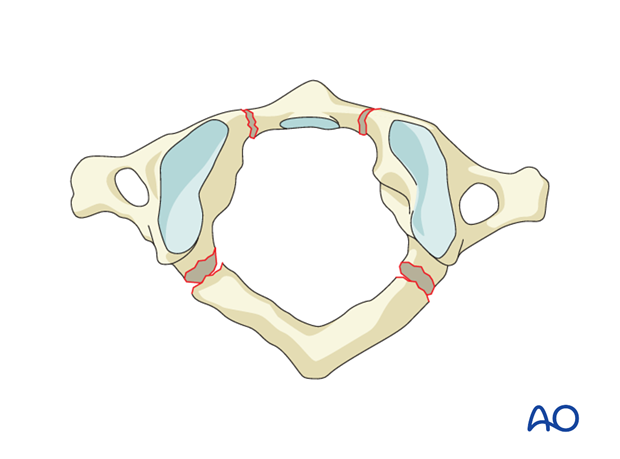
Transverse process injuries
Transverse process fractures are stable fractures and are treated nonoperatively with observation.
If the fracture involves the vertebral foramen, check for arterial injury.
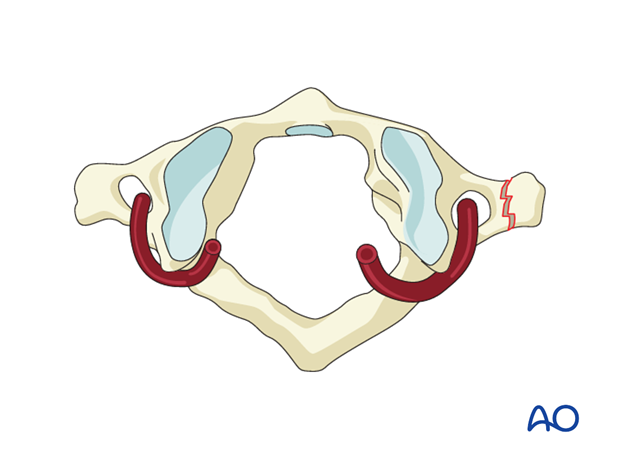
Lateral mass fractures
Unilateral lateral mass fractures may collapse and cause deformity or result in posttraumatic arthrosis. Therefore, primary fixation can be considered.
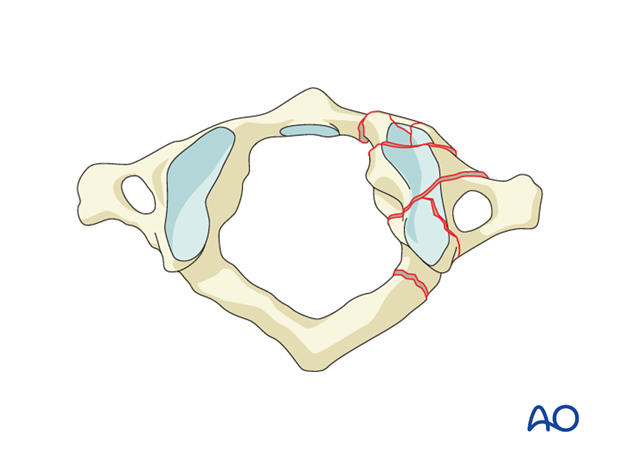
6. Region II: C1 ring and C1–C2 joint - Type B: Nondisplaced ligamentous injury
Type B injuries are transverse atlantal ligament insufficiencies, which may or may not be associated with fractures. There is no sign of C1–C2 displacement.
If a stress test shows displacement, then it is a Type C injury.
Treatment may be surgical or with halo vest in case there is bony avulsion injury.
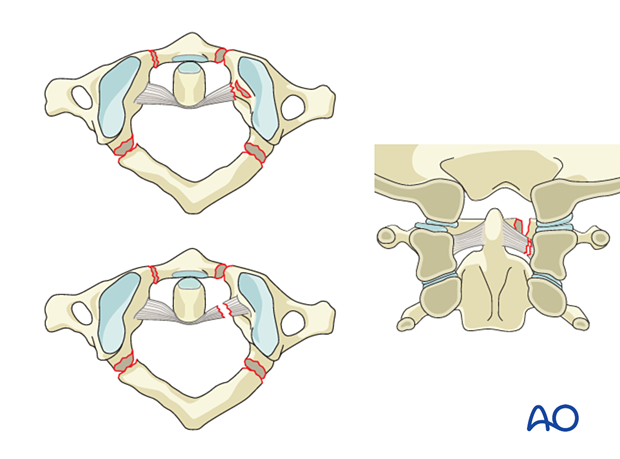
Displaced fractures with widening greater than 7 mm (rule of Spence: overhang on open-mouth odontoid view) suggest injury of the transverse atlantal ligament.
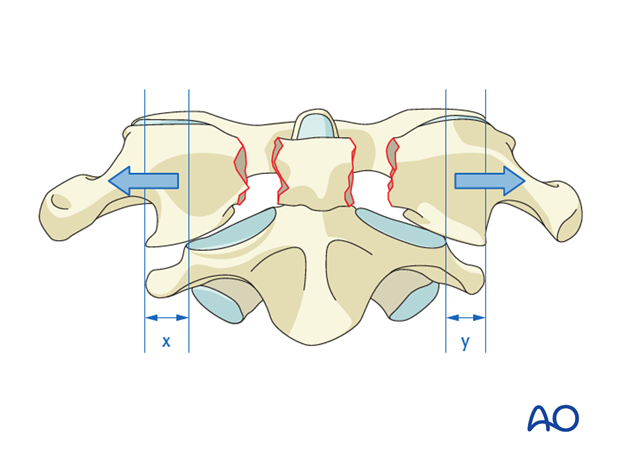
7. Region II: C1 ring and C1–C2 joint - Type C: Translation injury of the C1–C2 joint
Type C injuries are all injuries with atlantoaxial instability or displacement in any plane.
These injuries can be very unstable and may require operative management.
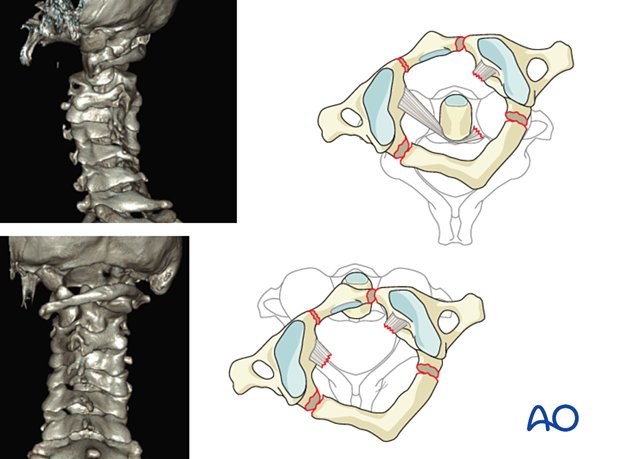
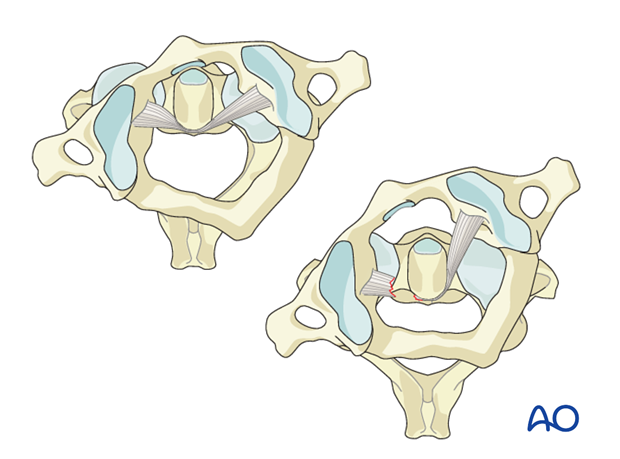
C1–C2 Rotatory subluxation
These are unique situations, which present in the pediatric age group after minor trauma or after throat inflammatory processes.
The transverse ligament is usually intact.
The treatment is conservative in acute cases with cervical traction and collar treatment. If closed reduction cannot be achieved, then open reduction and C1–C2 fusion would be indicated.
C1–C2 dislocations
C1–C2 dislocations may occur in traumatic accidents, but also with minor trauma, in congenital anomalies, or rheumatoid patients.
Axial CT images will show spinal canal narrowing due to the anterior dislocation.
The treatment is in general surgical with C1–C2 fusion.
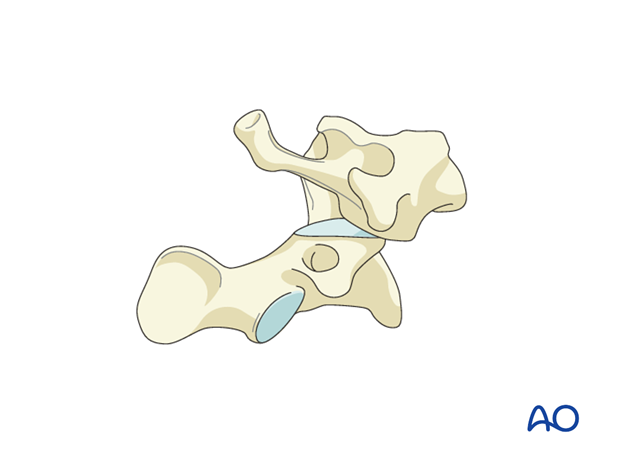
8. Region III: C2 and C2–C3 joint - Type A: Isolated bony injury of C2
Type A injuries are any C2 fractures (simple or multifragmentary) without significant ligamentous or discal injury.
This includes C2 fractures and odontoid fractures. C2 fractures are illustrated here.
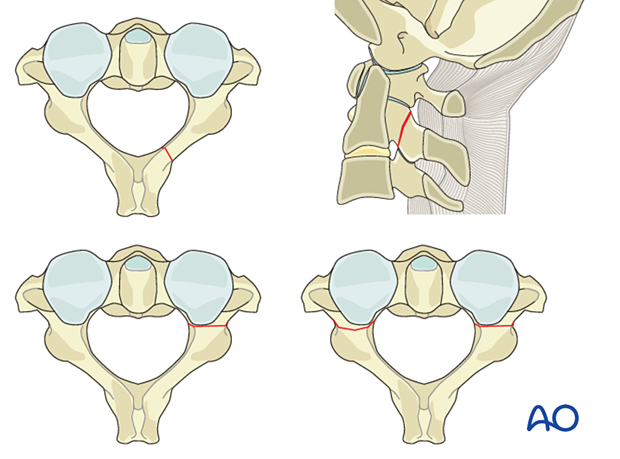
Odontoid fractures are illustrated here.
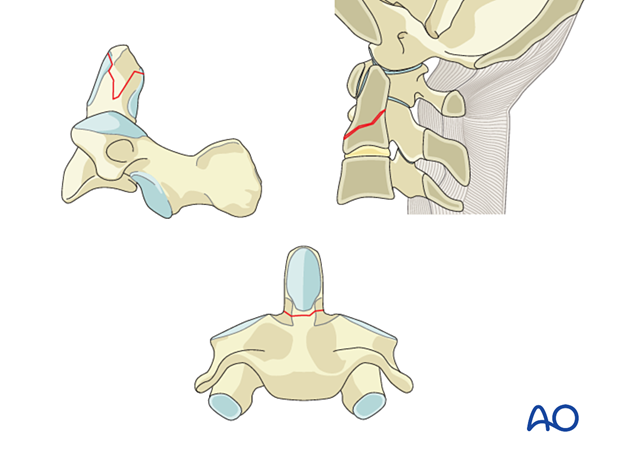
Odontoid fractures
Tip of the dens fractureThe tip of the dens is obliquely fractured on one side. This rare fracture may be due to a shear injury when the tip of the dens comes into contact with the rim of the foramen magnum, however, it can also represent an avulsion fracture of the alar ligament and must therefore be suspected to be part of an atlantooccipital dislocation.
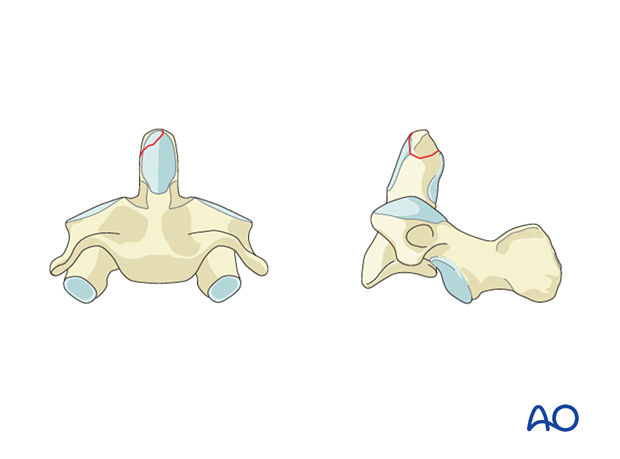
The fracture line is located in the odontoid peg itself, above the vertebral body of C2. The fracture surface is small and the fracture has a high nonunion rate when treated conservatively.
Most often the fracture is transverse but it may also be comminuted or oblique. The fractured odontoid process may be dislocated anteriorly or posteriorly, but the C1–C2 joint is not dislocated.
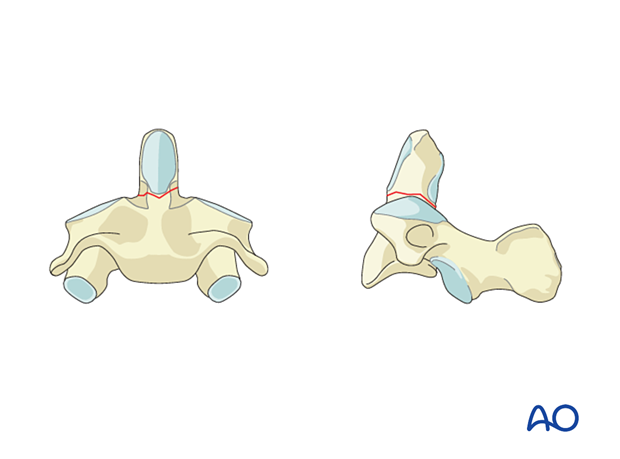
The fracture line is located in the vertebral body of C2 itself, underneath the odontoid peg. The fracture is in cancellous bone and therefore has a better healing potential with a lower nonunion rate when treated conservatively. The fracture often enters the lateral atlantoaxial joint on one or both sides and may create an intraarticular step. The fracture may also extend into the isthmus.
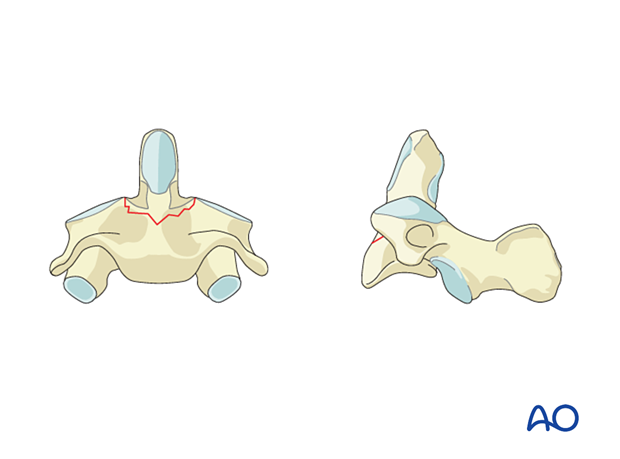
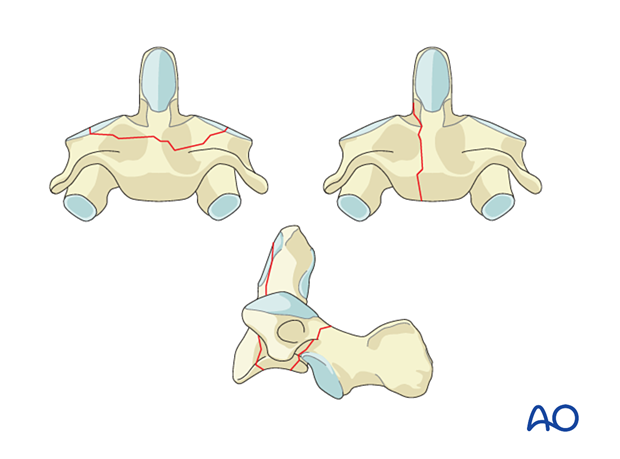
C2 Body fracture
C2 body fractures run either coronally, sagitally, or horizontally through the body.
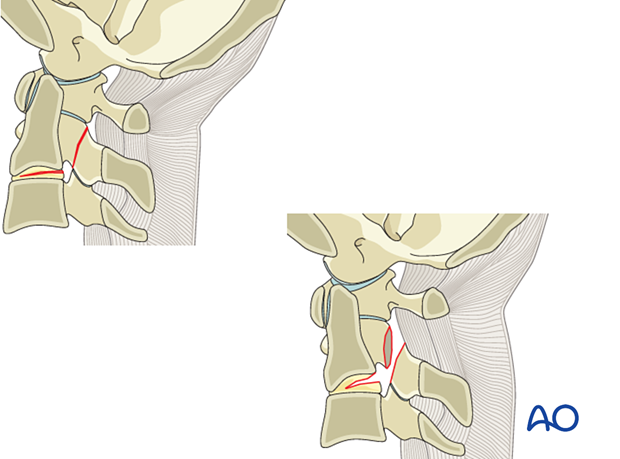
9. Region III: C2 and C2–C3 joint - Type B: Nondisplaced ligamentous injury
Type B injuries are tension band/ligamentous injuries, with or without bony injury.
This is the typical hangman fracture.
The posterior tension band is disrupted, as well as the disc.
However, there is no displacement between C2 and C3.
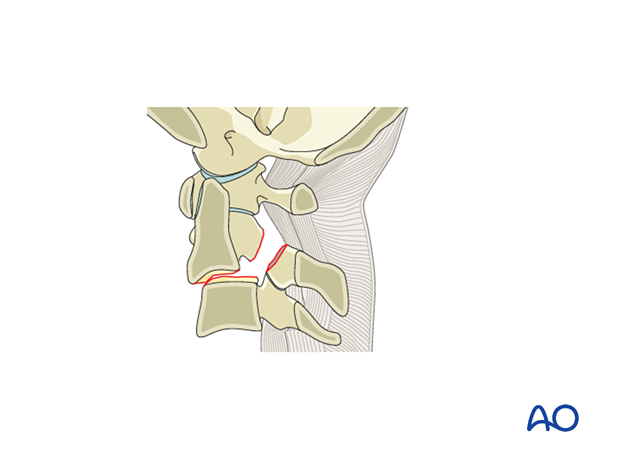
10. Region III: C2 and C2–C3 joint - Type C: Translation injury
Type C injuries are any injuries that lead to a displacement between C2 and C3.
This is the most severe type of hangman fracture with or without dislocation of the facet joints.
The posterior tension band is disrupted, as well as the disc.
11. Neurology
Neurology is assessed as shown on the grid following a neurological evaluation.
N0: Neurologically intact
N1: Transient neurologic deficit that has completely resolved by the time of clinical examination (usually within 24 hours from the time of injury)
N2: Radiculopathy
N3: Incomplete spinal cord injury
N4: Complete spinal cord injury
Nx: Unexaminable patient
+: Continued spinal cord compression
12. Modifiers
These modifiers are added to distinguish features that may impact treatment of a given fracture type.
M1: Injury at high risk of non-union with nonoperative treatment
- eg, Type II odontoid fracture
M2: Injury with significant potential for instability
- eg, midsubstance injury to transverse ligament
- eg, displaced C1 unilateral lateral mass fracture
- eg, >7 mm displacement of C1 lateral mass
M3: Patient specific factors affecting treatment
- eg, age, comorbidities, neurological status, smoking, other injuries, anklosing spondylitis
M4: Vascular injury or abnormality affecting treatment












